Top Benefits of Augmented Reality Knee Replacement
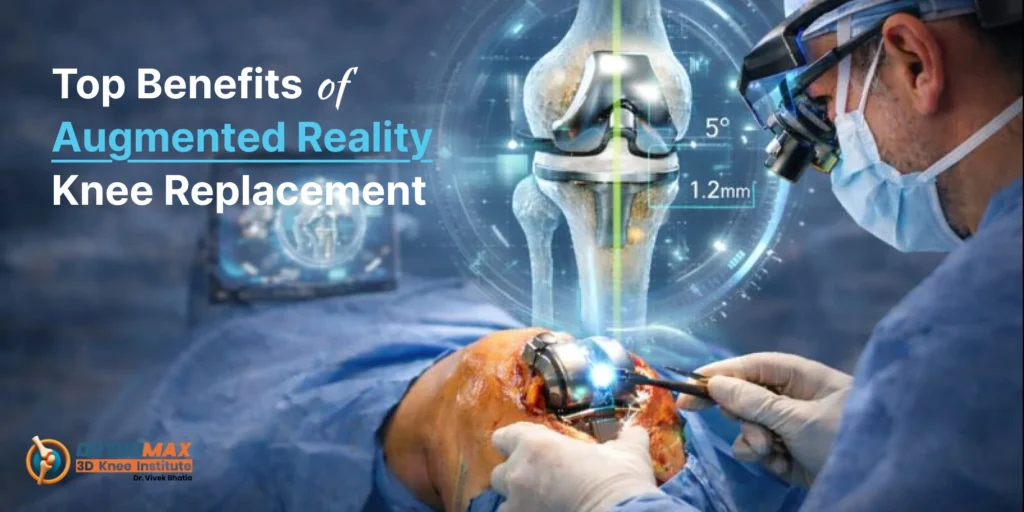
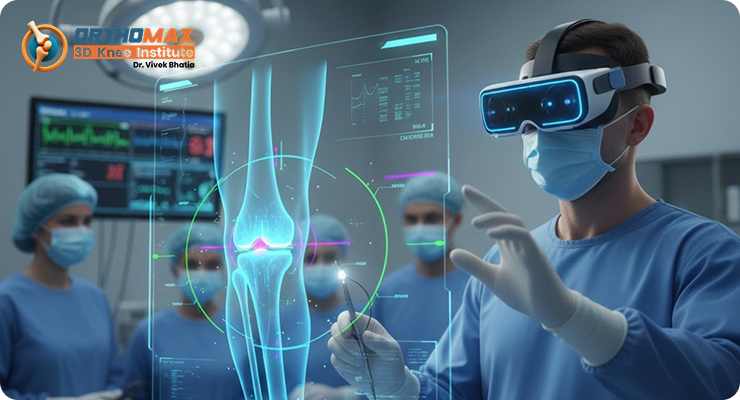
Top Benefits of Augmented Reality Knee Replacement Knee replacement surgery has transformed the lives of millions suffering from chronic knee pain, arthritis, and mobility limitations. Over the years, advancements in technology have significantly improved surgical accuracy, patient comfort, and recovery outcomes. One of the most promising innovations shaping modern orthopaedics is augmented reality (AR). By blending digital information with the real surgical environment, augmented reality knee replacement is redefining how surgeons plan and perform this complex procedure. Augmented reality is not science fiction anymore—it is a practical, surgeon-assisting technology that overlays real-time visual guidance during surgery. This advancement allows orthopaedic surgeons to perform knee replacements with greater precision, confidence, and consistency. Below are the top benefits of augmented reality knee replacement and why it is gaining popularity worldwide. 1. Enhanced Surgical Precision Precision is critical in knee replacement surgery. Even a small alignment error can impact joint function, implant lifespan, and patient satisfaction. Augmented reality systems provide surgeons with a real-time, three-dimensional view of the knee anatomy during surgery. This allows accurate placement of implants according to the patient’s unique bone structure. Unlike conventional methods that rely heavily on manual tools and estimation, AR technology guides the surgeon step by step. The result is more consistent accuracy, improved joint balance, and reduced chances of implant misalignment. 2. Personalized Treatment for Every Patient Every knee is different. Factors such as bone shape, degree of arthritis, ligament condition, and posture vary from person to person. Augmented reality enables patient-specific surgical planning by integrating preoperative imaging with intraoperative guidance. This personalized approach ensures that the knee replacement is tailored precisely to the patient’s anatomy rather than relying on a one-size-fits-all method. Customized alignment leads to better movement, increased comfort, and more natural-feeling knees after surgery. 3. Reduced Risk of Surgical Errors Traditional knee replacement techniques depend significantly on mechanical guides and the surgeon’s experience. While effective, they leave room for human error. Augmented reality acts as an additional layer of safety by continuously verifying alignment, angles, and implant positioning. By providing visual alerts and data during surgery, AR technology helps minimize deviations from the surgical plan. This reduces the likelihood of complications such as uneven joint loading, instability, or early implant failure. 4. Improved Implant Longevity One of the biggest concerns after knee replacement is how long the implant will last. Improper alignment is one of the leading causes of early implant wear and revision surgery. Augmented reality helps ensure optimal implant positioning, which distributes forces evenly across the joint. Better alignment means less stress on the artificial joint, reduced wear over time, and a longer lifespan for the implant. For patients, this translates into fewer chances of revision surgery and better long-term outcomes. 5. Faster Recovery and Rehabilitation Accurate surgery directly influences recovery speed. When implants are placed correctly and soft tissues are preserved, patients experience less postoperative pain and swelling. Augmented reality knee replacement supports minimally invasive techniques by guiding precise bone cuts and reducing unnecessary tissue trauma. As a result, many patients can start walking sooner, regain mobility faster, and return to daily activities with greater confidence. Shorter rehabilitation periods also improve overall patient satisfaction and quality of life. 6. Better Functional Outcomes The ultimate goal of knee replacement is not just pain relief but restored function. Augmented reality helps surgeons achieve better knee balance, alignment, and range of motion. This allows patients to experience smoother walking patterns, improved stability, and more natural knee movement. Patients often report better confidence while climbing stairs, standing for long periods, or engaging in light physical activities. These functional improvements make a significant difference in day-to-day life after surgery. 7. Consistency Across Surgical Outcomes One of the challenges in orthopaedic surgery is maintaining consistent results across different patients. Augmented reality standardizes critical steps of the procedure while still allowing surgeons to apply their expertise. This consistency benefits both experienced surgeons and those early in their careers. With AR guidance, outcomes become more predictable, reducing variations and improving overall surgical quality. Patients can feel more confident knowing that technology supports every stage of the operation. 8. Reduced Dependence on Bulky Instruments Conventional knee replacement often requires multiple mechanical alignment tools and jigs, which can clutter the surgical field. Augmented reality systems reduce reliance on these instruments by providing digital alignment guidance. This streamlined approach can shorten surgical time, reduce infection risk, and make the operating environment more efficient. Fewer instruments also mean less disruption to surrounding tissues. 9. Greater Confidence for Surgeons and Patients Augmented reality enhances surgeon confidence by providing continuous feedback during the procedure. Surgeons can verify decisions instantly rather than relying solely on visual judgment. This confidence is passed on to patients, who feel reassured knowing advanced technology is being used for their treatment. 10. Educational and Training Advantages Augmented reality is also a powerful teaching tool. It helps train surgeons by offering visual simulations and real-time guidance. This improves learning curves and promotes best surgical practices. Better training leads to better outcomes, ensuring that more patients benefit from high-quality knee replacement surgery performed with advanced techniques. 11. Supports Advanced Orthopaedic Care Standards The integration of augmented reality reflects a broader shift toward smarter, data-driven healthcare. It aligns with global standards of excellence and supports surgeons striving to deliver world-class outcomes. Patients seeking care from the best orthopaedic in Panchkula increasingly look for hospitals that adopt advanced technologies for improved safety and results. 12. A Future-Ready Solution for Knee Replacement Augmented reality is not a temporary trend—it represents the future of orthopaedic surgery. As technology evolves, AR systems will become even more intuitive, accurate, and accessible. This advancement complements other modern innovations and strengthens the overall success of knee replacement in Panchkula and beyond. Conclusion Augmented reality knee replacement is transforming the way knee surgeries are planned and performed. By enhancing precision, personalization, safety, and recovery, AR technology offers significant benefits for both patients and surgeons. From improved implant longevity to faster rehabilitation and better functional outcomes, augmented reality sets a